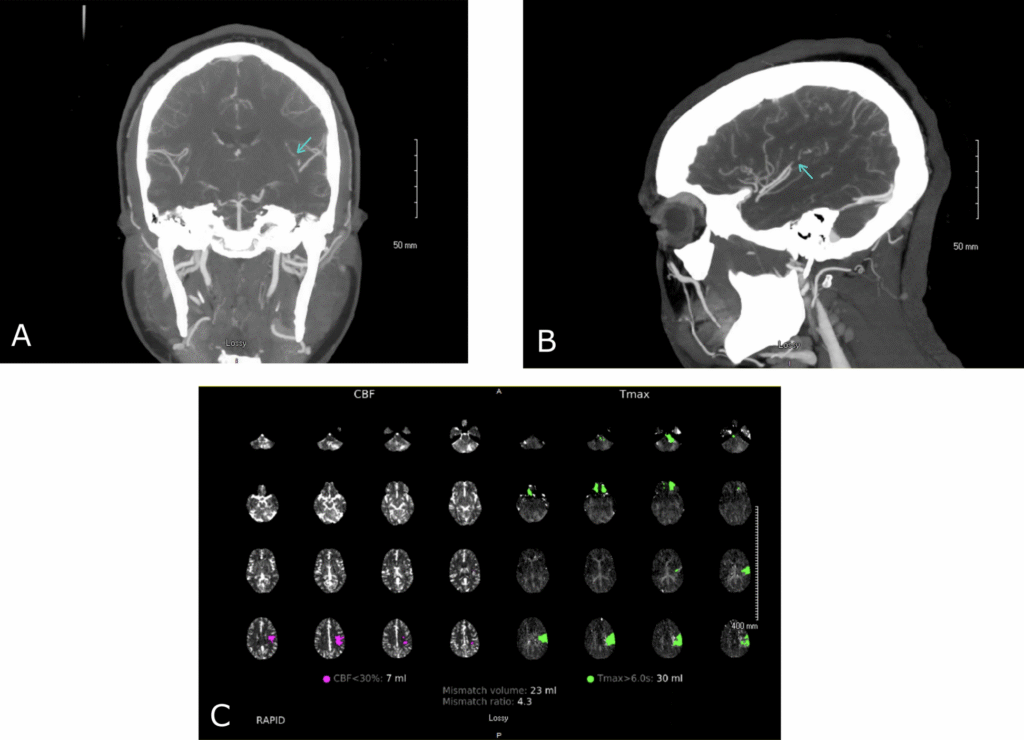
A recent case study has raised questions about the relationship between Epstein-Barr virus (EBV) infections and acute ischemic stroke (AIS) in young patients. The patient in question exhibited EBV-positive lymphoid proliferation, suggesting a potential connection with AIS, particularly due to her young age and lack of other significant stroke risk factors. Herpesvirus infections, including EBV, varicella zoster virus, and herpes simplex virus, have been implicated in the increased risk of ischemic stroke, notably in the pediatric and younger adult populations. Proposed mechanisms of this association include endothelial dysfunction, inflammatory cytokine release, and immune responses that may lead to vascular injury. Specifically, EBV may infect B lymphocytes, resulting in autoantibody production and potential coagulation issues that could elevate stroke risk.
While there have been isolated case reports of EBV-related strokes, comprehensive clinical trials on this topic remain scarce. Notably, a case described a 2-year-old girl developing an ischemic stroke related to EBV, characterized by elevated levels of inflammatory markers. Another case noted an adult suffering from brainstem hemorrhage due to EBV encephalitis, underscoring the virus’s potential to impact cerebral vasculature.
Given these insights, the report suggests that testing for EBV and other viral infections may be beneficial in young stroke patients lacking conventional risk factors. However, a definitive causal relationship remains uncertain, highlighting the need for further research in this area.
- Why it matters: Understanding the link between viral infections like EBV and ischemic stroke could inform clinical practices and improve patient management, particularly for young adults with unexplained stroke cases.
- The latest: Current literature indicates that further studies are needed to clarify the mechanisms linking EBV infection to increased stroke risk.
Source: https://jmedicalcasereports.biomedcentral.com/articles/10.1186/s13256-025-05641-0
Source: https://jmedicalcasereports.biomedcentral.com/articles/10.1186/s13256-025-05641-0